 
The procedure is performed for symptomatic gallbladder and bile duct disease. Surgical complications, including wound infections, adverse reactions to anesthetics, and injury to the liver, gallbladder, bile ducts, or neighboring organs, occur about 5% of the time. See: illustration. Acute, chronic, or acalculous cholecystitis (biliary inflammation that is not caused by gallstones), repeated episodes of biliary colic, biliary dyskinesia, gallstone pancreatitis, and occasionally cholangitis are indications for the procedure. The gallbladder does not usually need to be removed for asymptomatic gallstone disease. Patient care. Preoperative: The patient is informed about the procedure, including the need for drains, catheter, nasogastric tubes, etc., and taught about incentive spirometry, leg exercises, incision splinting, analgesia use, and other postoperative concerns. Postoperative: General patient care concerns apply. Vital signs are monitored and dressings are inspected. The patient is assessed for pain and for gastrointestinal and urinary function; analgesics and antiemetics are provided as needed. Fluid and electrolyte balance is monitored, and prescribed fluid replacement therapy is administered until the patient is permitted oral intake. The patient is encouraged to breathe deeply and to perform incentive spirometry to prevent atelectasis and impaired gas exchange. The patient is assisted with early ambulation and with splinting the abdomen when moving about or coughing. Peripheral circulation is evaluated, and venous return is promoted with leg exercises and elastic stockings or pneumatic hose as prescribed. If a laparoscopic approach is used, the patient will typically be discharged the day of or the day after surgery. Clear liquids are offered after recovery from general anesthesia, and the patient resumes a normal diet within a few days.

If an open incision is used, the patient is placed in a position of comfort; a nasogastric (NG) tube is frequently required to prevent abdominal distention and ileus, and is attached to low intermittent suction; and the volume and characteristics of drainage from the NG tube and any abdominal drains or T- tube are documented. Skin care and appropriate dressings are provided around any drain site. When peristalsis returns, the NG tube is removed as directed. Oral intake, beginning with clear liquids, is initiated. The T- tube may be clamped before and after each meal to allow additional bile to enter the intestine. 
Clinical recommendation Evidence rating References; First-line treatment of patients with cirrhotic ascites consists of sodium restriction (i.e., no more than 2,000. What is a kidney stone? Do I have a kidney stone? What are the symptoms of a kidney stone? Do all kidney stones cause pain? What causes a kidney stone? 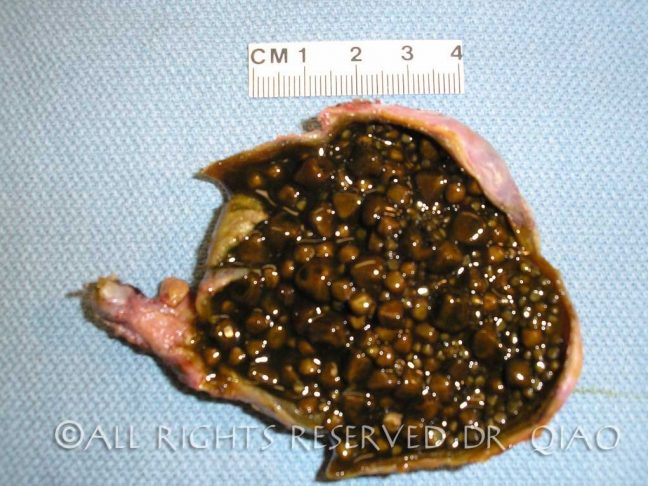   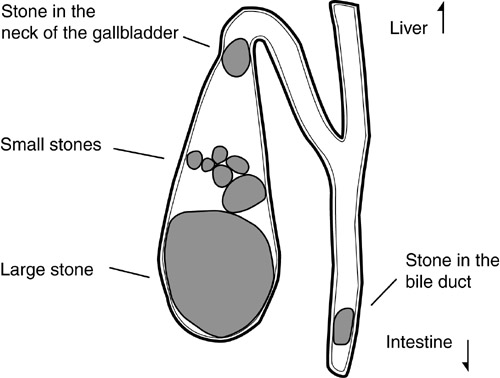 
Signs and symptoms of postcholecystectomy syndrome (fever, abdominal pain, and jaundice) and other complications involving obstructed bile drainage are reported; urine and stool samples are collected for analysis of bile content should any such complications occur. Discharge teaching for the patient and family includes wound care and T- tube care if appropriate (the T- tube may remain in place up to 2 weeks); the need to report any signs of biliary obstruction (fever, jaundice, pruritus, pain, dark urine, and clay- colored stools); the importance of daily exercise such as walking; avoidance of heavy lifting or straining for the prescribed period; and any restrictions on motor vehicle operation. Although diet is not restricted, the patient may be more comfortable avoiding excessive intake of fats and gas- forming foods for 4 to 6 weeks. Arrangements for home health follow- up or care may be necessary. The patient should return to the surgeon for a post- operative evaluation visit as scheduled. If gallstones were present, the patient is taught to reduce the risk of recurrence by maintaining normal body weight, exercising regularly, and eating three well- balanced meals daily, including fiber and calcium and avoiding alcohol and foods high in saturated fat. Weight loss, if needed, should be carried out gradually, and crash dieting discouraged. Surgery for gallbladder cancer in which the organ and surrounding tissues (the neighboring liver and regional lymph nodes) are removed. A polyp is an abnormal growth of tissue projecting from a mucous membrane. If it is attached to the surface by a narrow elongated stalk, it is said to be pedunculated.Removal of the gallbladder using a laser as a cutting tool, applied laparoscopically. This procedure may be inappropriate for patients with severe acute cholecystitis, a palpable gallbladder, or evidence of a stone in the common bile duct. The use of a laser as opposed to endoscopic electrosurgical instrument is according to the preference of the surgeon. Patient care. The nurse or surgeon explains to the patient that this type of surgery will not be used if the patient is pregnant or has had extensive abdominal surgery (because of concern for adhesions), severe acute cholecystitis, a palpable gallbladder, evidence of a stone in the common bile duct, or a bleeding problem. The patient is also told that the surgeon, using the endoscopic technique, will be able to remove the gallbladder without unsightly scarring, leaving only four (or less) small punctures, which reduces the risk for wound complications (infection, hematoma, separation). Risks for other complications (pneumonia, thrombophlebitis, urinary retention, and paralytic ileus) are also decreased because the procedure enables early mobility and may avoid use of parenteral analgesia. Patients will experience less pain and immobility, require less narcotic analgesia, be discharged on the same or on the next day, and be able to return to their usual activities (including work) within 7 days. Preoperative preparation, which usually is similar to that for any other abdominal surgery, is explained. Postoperatively, the patient is stabilized during a brief stay in postanesthesia and then is transported to a surgical observation unit. The patient is offered clear liquids (carbonated beverages are avoided because they may cause distension and abdominal pressure). If the patient tolerates liquids, the IV is removed, and the patient is offered a regular diet. Analgesics are administered orally as prescribed as soon as the patient can take liquids. A parenteral narcotic (which may cause drowsiness, reduced intestinal motility, and/or vomiting) is given only if the patient continues to feel pain after taking an analgesic. Once the patient is comfortable, he is helped to walk because early ambulation speeds recovery. The patient is usually fully awake and walking within 3 or 4 hr of arrival on the unit. If he experiences shoulder pain, a heating pad may be applied. The surgeon, however, usually removes the carbon dioxide at the end of the procedure to prevent this problem. The nurse evaluates the patient's readiness for discharge, which usually can occur if the patient is afebrile, walking, eating, and voiding, and has stable vital signs with no evidence of bleeding or bile leakage. To assess for the latter risks, the patient is observed for severe pain and tenderness in the right upper quadrant, an increase in abdominal girth, leakage of bile- colored drainage from the puncture site, a fall in blood pressure, and increased heart rate. The patient is instructed to keep the adhesive bandages covering the puncture site clean and dry. He may remove them the next day and bathe or shower as usual. The patient most likely will require little analgesia, but a prescription is given for use as needed. He is reminded to pace activity according to energy level. While no special diet is required, the patient may wish to avoid excessive fat intake and gas- forming foods for 4 to 6 weeks. He should return to the surgeon for follow- up evaluation as directed and report any vomiting, abdominal distention, signs of infection, and new or worsening pain.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
May 2017
Categories |
 RSS Feed
RSS Feed
